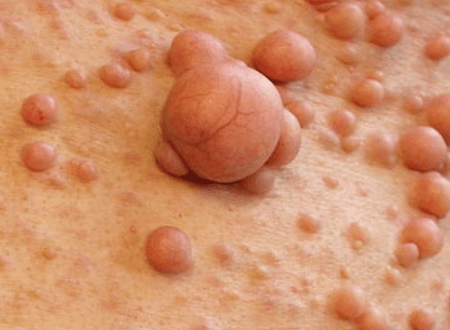
You may hear “NF” used in different ways, but when it refers to health it means a group of genetic conditions that cause tumors to grow on nerves and affect the skin, brain, and spinal cord. NF can range from mild skin changes and freckles to tumors that affect hearing, vision, or nerve function, and knowing the type—especially NF1 versus NF2—matters for diagnosis and treatment.
This article what is NF? This will help you understand the core medical facts behind NF, how doctors identify and classify the condition, and what treatment options and monitoring strategies exist to manage symptoms and risks. Armed with clear, practical information, you can recognize key signs, ask the right questions of clinicians, and follow evidence-based steps for care or family planning.
Medical Definitions and Core Concepts
You will find clear definitions, core features, warning signs, and common causes with risk factors to help recognize and respond to necrotizing soft-tissue infections quickly. Focus on rapid progression, severe pain, systemic toxicity, and which patients are at highest risk.
Understanding Necrotizing Fasciitis
Necrotizing fasciitis (NF) is a rapidly progressive bacterial infection that destroys fascia and subcutaneous tissue. It often begins after a break in the skin—minor cuts, insect bites, surgical wounds, or blunt trauma—and then spreads along fascial planes faster than superficial signs appear.
Pathology centers on bacterial toxins and host inflammation that cause tissue ischemia, necrosis, and sometimes gas formation. The process can lead to systemic inflammatory response, septic shock, and multi‑organ failure within hours to days if untreated.
Diagnosis relies on clinical suspicion plus supportive tests: imaging (CT/MRI) can show fascial edema or gas, laboratory risk scores (e.g., LRINEC) may help, and definitive diagnosis requires surgical exploration and tissue sampling.
Signs and Symptoms
Pain out of proportion to exam is an early and distinctive sign you should not ignore. Pain is often severe, constant, and extends beyond the visible skin lesion.
Skin findings may progress from erythema and swelling to blistering, dusky discoloration, anesthesia over necrotic areas, and crepitus if gas-producing organisms are present. Fever, tachycardia, hypotension, and altered mental status indicate systemic toxicity.
Laboratory abnormalities commonly include leukocytosis, elevated CRP, metabolic acidosis, coagulopathy, and acute kidney injury. Rapid deterioration over hours, rather than days, is typical and should prompt immediate surgical consultation.
Common Causes and Risk Factors
NF is polymicrobial in many cases (Type I) or caused by single virulent organisms such as group A Streptococcus or Vibrio vulnificus (Type II/III). Mixed aerobic–anaerobic infections often follow gastrointestinal or perineal sources; monomicrobial cases often follow skin breaches.
Key risk factors that increase your likelihood of NF include diabetes mellitus, chronic liver disease, peripheral vascular disease, immunosuppression, obesity, and recent surgery or trauma. Intravenous drug use and advanced age also raise risk.
Environmental exposures matter: seawater or raw seafood contact increases risk of Vibrio infections; recent bowel perforation or perianal procedures increase risk of polymicrobial perineal NF (Fournier gangrene). Identify these risks early to prioritize assessment and urgent intervention.
Treatment Approaches and Prevention
You will encounter a mix of diagnostic tests, targeted and general treatments, and practical prevention measures to reduce risks and detect complications early. These approaches aim to control symptoms, preserve function, and monitor for malignant change.
Diagnostic Procedures
You receive diagnosis through clinical exam, family history, and targeted testing. A neurologic and dermatologic exam documents café-au-lait spots, neurofibromas, Lisch nodules (eye), and focal neurologic deficits.
Genetic testing for NF1, NF2, or SMARCB1/LZTR1 (schwannomatosis) confirms the diagnosis in many cases and helps with family planning. Testing uses blood or saliva samples and sequencing plus deletion/duplication analysis when indicated.
Imaging localizes and characterizes tumors. Use MRI of brain and spine with contrast for suspected optic pathway gliomas, vestibular schwannomas, or plexiform neurofibromas. Consider CT when bone involvement or calcification is a concern.
You should undergo baseline and interval surveillance tailored to your NF type and age. For children with NF1, periodic developmental and vision screening is essential; for NF2, audiology and MRI follow-up are central.
See also: Furnace Maintenance Guide: Seasonal Checks, Common Repairs, and Energy Savings
Medical and Surgical Interventions
You will receive treatments chosen by symptom, tumor type, location, and growth behavior. Observe small, asymptomatic lesions with scheduled imaging and clinical checks.
Medications include targeted therapies (for example, MEK inhibitors for growing plexiform neurofibromas) and conventional options such as analgesics, antiemetics, or steroids for symptom control. Chemotherapy, radiation, or targeted agents treat malignant transformation or specific tumor types when indicated.
Surgery removes or debulks tumors causing pain, neurologic compromise, or airway/organ compression. Neurosurgeons, ENT, ophthalmology, and plastic surgeons coordinate care for complex resections. Risks include neurologic deficit and scarring; weigh benefits against functional outcomes.
Rehabilitation and supportive care preserve function and quality of life. This includes physiotherapy, pain management (including neuropathic agents), occupational therapy, educational support for learning differences, and psychosocial services. You may need multidisciplinary clinics for coordinated decision-making.
Prevention Strategies
You cannot prevent inherited NF mutations, but you can reduce complications through surveillance and lifestyle choices. Keep recommended imaging and clinical follow-up to detect tumor growth early when interventions are safer and more effective.
Genetic counseling helps you understand inheritance, recurrence risk, and reproductive options such as prenatal testing or preimplantation genetic testing (PGT). Discuss these options with a genetics professional before conceiving.
Minimize modifiable risk factors that worsen outcomes: avoid tobacco, manage blood pressure and metabolic health, and promptly treat infections or injuries near affected nerves. Protect skin from trauma and monitor any rapid changes in lesions.
Create an individualized care plan with your specialists. Use written action items for new symptoms (rapid pain increase, new neurologic signs, sudden growth or bleeding) so you seek timely evaluation.